If Nurses Run the Floor, Why Aren’t They Designing It?

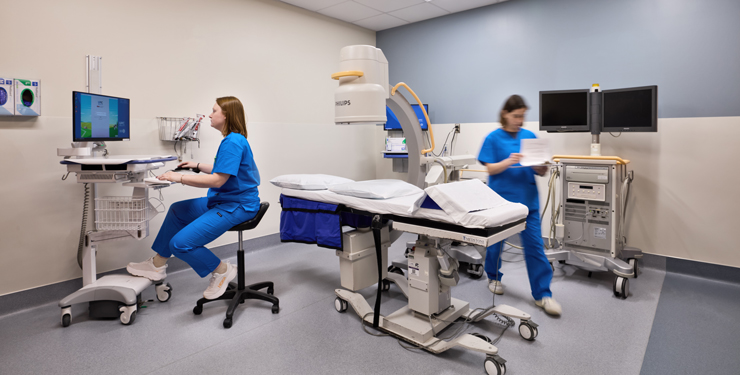
In the world of healthcare, nurses understand how to provide effective, patient-centered care. They interface directly with patients on a regular basis, sometimes more than doctors. But when it comes to the design of healthcare facilities, nursing input is lacking.
For ideal outcomes in critical environments like healthcare, listening to key stakeholders like nurses is essential.
Nurse Participation Directly Influences Design Success
Delivering an optimal patient experience is a shared objective in healthcare environments. This often drives new construction and renovation – but achieving it is complex and multifaceted. An essential factor influencing success? The degree to which frontline caregivers, particularly nurses, are meaningfully engaged in the design process.
This blog collects key points from our white paper research on the benefits of engaging nurses to create satisfactory, patient-centered healthcare design.
As the foremost experts on how healthcare spaces function (and fail), nurses can offer valuable insights into their design. Unfortunately, they’re not often consulted and rarely part of the decision-making process. We reached out to nurses to hear their direct perspectives and understand the current state of nurse participation in healthcare design.
Our survey was distributed nationally through a nurse research panel and received over 250 responses. The survey included qualitative and quantitative questions, including, among others:
- Participation in design projects, including types of projects
- Access and barriers to participation
- Benefits of including nurses in the design process
The Current State of Nurse Participation
The survey revealed that while nearly nine in ten nurses (86%) believe nurse inclusion in design is very or extremely important, only about one in ten (8.5%) feel they are mostly or fully included in these processes.
Participation usually occurs at the beginning, during visioning or discovery phases. Nurses are invited to presentations, complete surveys, or participate in early focus groups. While these formats offer exposure, they rarely extend to decision authority. More meaningful hands-on involvement, such as mock-ups, simulation, or committee participation, is far less common.
When they’re engaged, nurse contributions focus on the core mechanics of safe and reliable care – workflow and operational efficiency, patient safety, and infection prevention. But too often, these insights are solicited late in the process, after design concepts have been established.
The nursing profession is directly affected by spatial design for healthcare operational efficiency. When participation in the design process does occur, there are several benefits:
- Better alignment between design intent and clinical reality
- Smoother activation
- Higher staff confidence
- Sense of ownership and pride for nurses
Among nurses who participated in a project design process, 65% were satisfied or very satisfied with their experience, and 60% were satisfied with the resulting project. By contrast, for those who did not participate, two-thirds (66%) were dissatisfied or very dissatisfied with their lack of inclusion, and fewer than 20% reported satisfaction with the outcome. Statistical analysis confirmed a strong positive correlation (≈ 0.75) between satisfaction with participation and satisfaction with project outcome. A correlation of this magnitude indicates that when nurses are meaningfully engaged in the design process, satisfaction with the resulting environment rises substantially.
When nurses feel their expertise is acknowledged and their input incorporated, they are far more likely to believe the final environment supports safe, efficient, and effective care.
For healthcare leaders, this finding reframes participation. Engagement is a measurable driver of project success. Hospitals that embed nurses' voices throughout the design process experience higher satisfaction, stronger adoption of new spaces, and fewer costly revisions.
Bringing Nurses and Their Expertise to the Table
If nurse participation has such substantial benefits, why is it so limited? The data makes it clear: lack of access. Among nurses surveyed who had never participated in design, 93% said they were never asked. The data suggests that the participation gap is not driven by reluctance from nurses, but by the absence of structured processes for including them.
Many nurses are unsure whether they’re allowed to participate or assume that participation is reserved for managers. Others cite a lack of coverage or time. Even when nurses are invited, they’re often asked for feedback after design decisions have already been made.
Additionally, scheduling plays a role in keeping nurses out of the design process. Design meetings are often held during day shifts, excluding night and weekend staff. Input channels vary widely, and follow-up is rare. Without transparency about how feedback is used, trust erodes.
These experiences create skepticism about whether engagement will have any real impact on the design. Nurses want their perspectives meaningfully used – not just a tick on a checkbox. Most systems lack a reliable, consistent method to incorporate nursing input that feels authentic and consequential.
When Nurses Are Involved, Outcomes Are Better
The frontline perspective nurses bring provides a direct understanding of how design affects care delivery in real time. They are uniquely positioned to identify design change details that would streamline workflows and reduce risk. These can include:
- Medication room placement
- Charting locations
- Sightlines from team bases
In this survey, nurses linked their inclusion to efficiency and safety. Adjacency improves response times. Sightlines impact safety. Storage, noise, and lighting all affect staff performance and patient experience. Nurse participation leads to smoother transitions at occupancy, faster adaptation to new layouts, and fewer operational surprises.
The conclusion is straightforward: Build spaces with nurses, not merely for them.
5 Key Implications of Co-Design in Healthcare
Healthcare systems must move to structured collaboration between nurses and other stakeholders, incorporating input into the final product.
1. Design Outcomes Mirror Participation Quality
Projects where nurses meaningfully participate show higher satisfaction with both the process and the built result. Nurse engagement should be treated as a leading indicator of project success, on par with safety, schedule, and budget metrics.
2. Inclusion Gaps Stem from Process, Not Attitude
93% of nurses who were not involved in the design process said they were never asked to participate. The solution is structural, not motivational. Invitations must be systematic, not situational.
3. The Wrong Participation Windows Limit Design Value
Nurses are often engaged early in visioning or programming, but rarely during design phases when spatial, operational, and safety decisions are finalized. True co-design requires involvement in mock-ups, simulations, committee reviews, and post-occupancy evaluations.
4. Participation is an Operational Safety Measure
In the survey, responding nurses link their inclusion to workflow efficiency, error reduction, and infection control, all core operational outcomes. Including nurses reduces rework and downstream change orders while improving healthcare outcomes.
5. Measuring Space Performance Closes the Loop
Spaces need to be tested under real conditions to verify design decisions. Embedding measurement completes the feedback loop and transforms design into an ongoing learning process. Involving nurses in post-occupancy evaluations captures real-world performance and refines space over time.
Next Steps for Improving Operational Efficiency in Healthcare
By establishing structured, transparent mechanisms for nurse inclusion throughout the design process, organizations can reduce inefficiency, strengthen safety, and create environments that perform as intended.
Translating nurse insight into better healthcare environments requires more than occasional consultation. It requires a structured framework that embeds frontline expertise throughout the design lifecycle.
The following recommendations outline steps to embed this collaboration into policy, processes, and culture.
Governance and Policy
- Institutionalize the “ask”: Make nurse invitation and participation a required component in project charters, RFPs, and A/E contracts.
- Establish a Nurse Design Council: Create rotating membership across units and shifts, including staff, advanced practice, and leadership roles.
- Measure participation: Track invited attended influenced at each phase as a project KPI.
Participation Framework
- Pre-Design: Two-way Q&A sessions; publish who was invited.
- Design: Mandatory mock-ups and scenario testing with shift-safe scheduling and funded iteration time.
- Construction: Define committee decision rights and provide coverage/backfill for nurse participants.
- Occupancy: Create an ongoing Post-Occupancy Evaluation (POE) process led by nurses within 90 days of occupancy.
Representation & Equity
- Ensure quota-based representation by role, unit, and shift.
- Provide asynchronous participation options (surveys, digital forms, comment cards, analog sticker-dot voting) for off-shift staff.
- Include representation parity in performance dashboards.
Transparency & Trust
- Share concise “You said We did” summaries.
- If recommendations cannot be implemented, communicate why and note compensating design actions.
- Publicize nurse participation data to build accountability and organizational pride.
Get Started: Design with Nurses in Mind
Engaging nursing staff in the design process translates into decisions that improve operational effectiveness and patient outcomes.
BHDP, an award-winning, international, multi-disciplinary firm, is recognized for innovative and inspiring solutions across a spectrum of services, including strategic consulting and applied research. Our team of experts helps bridge the gap between theory and practice, providing the necessary groundwork for innovations that directly influence the design of places where people live, work, and grow.
Need to make sure your healthcare facility is designed to optimally serve nurses and patients alike? Fill out the contact form below to see how BHDP can help.
Author
Content Type
Date
March 17, 2026
Market
Topic
Healthcare Design